Sunday, January 1, 2012
What’s Really Driving Opioid-Related Death Rates?

By guest author, Bob Twillman, PhD, FAPM
On November 1, 2011, the Centers for Disease Control and Prevention (CDC) issued a Morbidity and Mortality Weekly Report (MMWR) titled “Vital Signs: Overdoses of Prescription Opioid Pain Relievers — United States, 1999-2008” [CDC 2011a]. In this document, CDC researchers report finding that opioid analgesics were involved in 14,800 prescription-drug overdose deaths in 2008. They assert that the per capita rate represented by this number is nearly 4 times the rate in 1999; note, however, they do not provide the actual data to support this, although examination of a graph in figure 2 of the MMWR document appears to justify this calculation [also see graph in prior UPDATE here].
CDC also presents data showing that per capita opioid analgesic sales increased in a roughly parallel manner during that interval. The authors of the report carefully avoid saying that the increase in opioid-analgesic-related deaths is caused by increased opioid analgesic sales (perhaps because they do not actually test this relationship statistically), but the clear implication is that increased prescribing is leading to increased sales and deaths. In contrast, an examination of other available data may not be especially supportive of this implication and suggests at least 6 alternative explanations.
Relevant Data: National Survey on Drug Use and Health (NSDUH)
The NSDUH is a national survey conducted every year by the Substance Abuse and Mental Health Services Administration [SAMHSA 2011], an agency of the US Department of Health and Human Services. Results from this survey are available [here] from 1998 (when it was called the National Household Survey on Drug Abuse) through 2010. Two key estimates in this survey related to the MMWR assertion are: (A) rates of “non-medical use of pain relievers,” defined as using a prescription pain reliever that was not prescribed for the respondent, or only for the experience or feeling it caused; and, (B) rates of DSM-IV-TR-diagnosed opioid abuse and opioid dependence.
Regarding these data, a couple of considerations must be noted. First, nonmedical use, as defined in NSDUH, may represent at least two distinct phenomena: a) use of opioid analgesics that had been prescribed to someone else by the respondent to treat their own pain (or, “medical misuse”), and b) use to alter one’s mood or mental status (“recreational use”). Second, in DSM-IV-TR — or, the Diagnostic and Statistical Manual of Mental Disorders, 4th edition, text revision, from the American Psychiatric Association — opioid abuse and opioid dependence are subtypes of substance use disorders, and are the nearest approximation to what others call “addiction.”
The simplest explanation for a link between opioid prescribing and overdose deaths would involve increases in nonmedical use and/or addiction resulting from the increased prescribing. CDC reported sharp increases in opioid analgesic sales between 1999 and 2010 in the MMWR document, so under this hypothesis, we would expect nonmedical use (NMU) and opioid use disorders (OUD) to also increase sharply during that interval. NSDUH data did not separately track prescription opioids until 2002, so we can only examine data from 2002 through 2010.
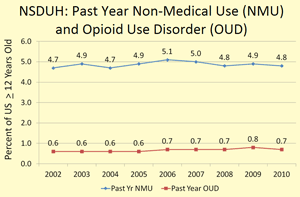
Looking at these data (Figure at right) it seems apparent that rates of NMU and OUD among Americans 12 years old and older are remarkably stable throughout this 9-year time period. It is certainly good news that neither NMU nor OUD were increasing, but it complicates explanations for increased opioid-related overdose deaths. Six alternative explanations are proposed below; although, there may be others and these 6 are decidedly not mutually exclusive. Readers are invited to add more alternatives in comments to this article.
Alternative Explanation #1: Dependent Variable Problems
The first alternative is that the dependent variable — that is, overdose deaths involving opioid analgesics — is unreliable and/or subject to reporting biases. CDC gathers these data from death certificates filed with state agencies across the country. Three possible difficulties with the quality of these data are immediately obvious:
- In the MMWR document, opioid-related overdose deaths are noted to include deaths of any intent, including unintentional, suicide, homicide, or undetermined. Suicide and homicide are very different from unintentional overdose deaths, and the ‘undetermined’ category undoubtedly includes some combination of the other three in unknown proportions. Thus, we do not know how many were truly unintentional overdoses.
- There is no standard definition of an opioid-related overdose death. CDC itself apparently recognizes this, as it has issued a call for assistance in developing consistent standards [CDC 2011b]. Lack of a standard definition could lead to idiosyncratic reporting of this cause of death, even among highly qualified medical examiners.
- Many death certificates are completed by county coroners. Qualifications for county coroners vary widely across the United States and, in some jurisdictions, coroners are not even required to be medical professionals. Public television station WGBH highlighted this issue in a Frontline episode entitled “Post Mortem: Death Investigation in America” [available for viewing here]. It is plausible that increased media attention to prescription medication misuse and overdose deaths could influence coroners — especially those who are not forensic pathologists or even physicians — to more likely report a suspicious death as being due to an overdose of opioid analgesics.
Together, these 3 concerns cast considerable doubt over whether the observed dependent variable — opioid overdose deaths — is accurate and reliable. If it is not, then the whole discussion is null and void. For the sake of argument, though, let’s assume there is at least a kernel of truth in the increased opioid overdose death rates and move on.
Alternative Explanation #2: Greater Use of Riskier Medications
If it is not the case that more people are engaging in NMU of opioid analgesics, as the NSDUH data clearly indicate, the explanation for increased mortality most likely lies in some change in patterns of behavior among the roughly 4.8% to 4.9% of Americans 12 or older who are “nonmedical users” of opioids. One possible change is a shift in the specific opioid analgesics used.
As availability of specific medications changes in response to changes in prescribing patterns, and as tamper-deterrent formulations of existing medications become more prevalent, it is possible that nonmedical users are turning to ”riskier” medications, such as methadone. The unique pharmacokinetic properties of methadone make it much more difficult to safely use both therapeutically and nonmedically, and it is possible that this risk translates into a higher death rate among those using it nonmedically.
Alternative Explanation #3: Lethal Doses of Medications
It is not clear if there are data to support this notion, but perhaps those engaging in NMU are using the same medications, but at higher potency. A subtle aspect of this problem is related to the fact that most individuals who misuse prescription opioids do so by swallowing them intact [Rosenblum et al. 2007]. If there is a trend away from misusing longer-acting or controlled-release formulations and substituting instead immediate-release versions of the same drugs at roughly the same dose, the effect could be two-fold: 1) shorten the time in which a maximum concentration of drug is reached in the blood (t-max), and 2) increase the maximum total concentration in the blood (c-max) — thus producing greater respiratory depression and a greater likelihood of death.
Alternative Explanation #4: More Frequent Use of Concomitant CNS Depressants
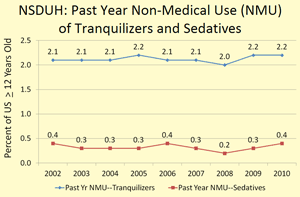
Most fatal overdoses involving opioid analgesics entail the simultaneous use of other central nervous system depressants, such as barbiturates, benzodiazepines, and/or alcohol [Hall et al. 2008], and there could be a greater tendency to use opioid analgesics in conjunction with these other drugs. However, NSDUH data (Figure at right) do not support the notion of increased NMU of tranquilizers (primarily benzodiazepines) or sedatives (including barbiturates), so this alternative explanation requires further scientific investigation.
Alternative Explanation #5: More Frequent Episodic Rather Than Daily Use
People who use opioid analgesics on a daily basis are likely to develop tolerance to their effects, including analgesia, euphoria, and respiratory depression. All that is known about individuals engaging in NMU of opioid analgesics is that a small proportion (those with an Opioid Use Disorder, or OUD) are likely to be using them on a very regular basis, and are more likely to be opioid tolerant. It is possible that those engaging in NMU without developing OUD are increasingly “bingeing” in such use, exposing themselves to greater mortality risks because their tolerance to respiratory depression is diminished compared with those who use opioids regularly.
Alternative Explanation #6: Shifts in the Type of NMU
As outlined above, there are two primary types of nonmedical use, or NMU: medical misuse and recreational use. Perhaps the observed increases in opioid analgesic prescribing means that more people are having their pain controlled through legitimate means, thereby reducing the number of medical misusers. If that is true (and it would represent good news), then the stable rate of NMU would suggest that most of those aberrant behaviors are associated with recreational use, and that more people are engaging in recreational use.
The remaining medical misusers may be taking doses of opioid analgesics sufficient to confer tolerance to respiratory depression but not enough to provide adequate analgesia. Additionally, it has been observed that pain is a natural antagonist to respiratory depression [Hanks et al. 1981; AAPM/APS 1997; Eriator 1998]. All of this suggests that it is recreational users who may be at greatest risk of fatal overdose, and their increasing numbers may be fueling the increased opioid-related death rate.
The Implied Research Agenda
CDC, in the MMWR document that spurred this discussion, proposes a number of policy solutions for the reported problem of increased opioid-related deaths. However, it is unclear that the solutions are based on a clear understanding of what is producing the problem, and it is equally unclear if the solutions would be effective.
What is clear is that there appears to be an opioid-overdose problem (assuming Alternative Explanation #1 regarding faulty case-definitions does not explain away the rise in opioid deaths). Just as a physician faced with a patient experiencing elevated blood pressure must work through a differential diagnosis to find the appropriate treatment, CDC and the medical community must work through a differential diagnosis of the overdose mortality problem to find appropriate solutions.
The 6 alternative explanations above comprise a list of alternate “diagnoses,” which must either be ruled out or accepted, and each of those may suggest different policy responses. Efficient and effective efforts to solve this problem can only be undertaken if we fully understand the nature of the problem. Let’s first get the proper research done, so we can move on with solving the problem.

About the Author: Bob Twillman, PhD, FAPM, is the Director of Policy and Advocacy for the American Academy of Pain Management. A 2011-2012 Mayday Pain & Society Fellow, he is also a Clinical Associate Professor of Psychiatry and Behavioral Sciences at the University of Kansas School of Medicine. Dr. Twillman practiced as a clinical psychologist in academic medical centers for 20 years, primarily in the areas of psycho-oncology and pain management.
REFERENCES:
> AAPM/APS (American Academy of Pain Medicine, American Pain Society). The use of opioids for the treatment of chronic pain. A consensus statement from the American Academy of Pain Medicine and the American Pain Society Quality of Care Task Force. Clin J Pain. 1997;13:6-8.
> CDC (US Centers for Disease Control and Prevention). Vital signs: Overdoses of prescription opioid pain relievers—United States, 1999-2008. Morbidity and Mortality Weekly. 2011a;60(43):1487-1492 [PDF available here].
> CDC (US Centers for Disease Control and Prevention). Opiate and opioid intoxication. RFQ: Development of a position paper that would provide guidelines in determining deaths from opiate and opioid intoxication. 2011b [access here].
> Eriator I. Narcotic analgesics for chronic pain management. Cur Rev Pain. 1998;2:193-200.
> Hall AJ, Logan JE, Toblin RL, et al. Patterns of abuse among unintentional pharmaceutical overdose fatalities. JAMA. 2008;300(22):2613-2620.
> Hanks GW, Twycross RG, Lloyd JW. Unexpected complication of successful nerve block. Morphine induced respiratory depression precipitated by removal of severe pain. Anaesthesia. 1981;36:37-39.
> Rosenblum A, Parrino M, Schnoll SH, et al. Prescription opioid abuse among enrollees into methadone maintenance treatment. Drug Alcohol Depend. 2007;90(1):64-71.
> SAMHSA (Substance Abuse and Mental Health Services Administration). National Survey on Drug Use and Health (NSDUH). Rockville, MD: Substance Abuse and Mental Health Services Administration; 2011 [access here].