Sunday, March 14, 2010
NSAID Dangers May Limit Pain-Relief Options
With recent concerns about risks of opioid and acetaminophen analgesics, the inherent dangers of nonsteroidal anti-inflammatory drugs (NSAIDs) seem to have escaped attention. Yet, as a class, ubiquitous NSAIDs may be the most hazardous. The dilemma is that an over-emphasis on risk avoidance could result in having fewer analgesic options remaining for the millions of persons with daily pain.
The NSAID class of drugs includes traditional nonselective NSAIDs — like aspirin, ibuprofen, naproxen, and others — as well as selective COX-2 inhibitors, like celecoxib. In a recent blogpost [available here] we noted that NSAIDs are widely prescribed and many are accessible over-the-counter (OTC), so they are used by millions of persons to treat fever, inflammation, and acute or chronic pain. While there can be very serious risks associated with these agents, only a limited amount of high-quality evidence exists to guide their safe use. At the same time, the U.S. FDA is considering new restrictions, some quite severe, on acetaminophen products [see prior blogpost discussion here] and on opioid analgesics via REMS initiatives [blogposts here and here]. Furthermore, as we recently discussed [here], in many parts of the world access to opioid analgesics already is being denied to millions of patients who would benefit. Taken together, these developments may compel greater reliance on NSAID use, even though there is insufficient awareness of the risks or knowledge of safety-enhancing strategies.
NSAIDs Risks Greater Than Many Realize
A recently-developed website from the American Gastroenterological Association (AGA) — called “Connect to Protect” [http://www.connecttoprotect.com/] — attempts to educate healthcare providers and consumers about gastrointestinal (GI) complications associated with NSAID use and ways to manage those risks. It should be acknowledged that funding for the site was provided by a grant from Horizon Therapeutics, Inc., a manufacturer developing combination products containing NSAIDs with high dose famotidine, a potent H2-antagonist. The site notes and references some alarming data:
-
- An estimated 60 million Americans regularly use NSAIDs, resulting in clinically significant upper GI complications in up to 2% of users (1.2 million cases).
-
- More than 80% of patients developing GI complications have no prior symptoms or warning signals.
-
- GI hemorrhages due to NSAID use result in up to 120,000 hospital admissions annually.
- Estimates are that more than 16,500 persons die from NSAID-related GI adverse events each year in the U.S. alone.
Actually, as astonishing as that 16,500+ yearly mortality figure may seem, the data originally reported by Wolfe et al. [1999], which they described as a “silent epidemic,” included only deaths associated with NSAID prescriptions for rheumatoid arthritis and osteoarthritis, did not take into account deaths from OTC NSAID products, and cardiotoxic influences of NSAIDs on mortality were not fully recognized at that time. In comparison, as we previously noted [here], available data from the U.S. indicate that fatalities associated with acetaminophen (or APAP) are low; in 2005, there were about 2,700 APAP-associated poisoning cases and 460 deaths. That same year, there were 8,500 deaths associated with prescription opioid analgesics [NDIC 2009]. Comparable mortality data for NSAIDs in 2005 do not appear to be available; however, there is every reason to believe that the 16,500+ figure from 1999 would be overly conservative if applied to 2005, since more NSAIDs became available via OTC distribution and deleterious affects of NSAIDs on cardiovascular health have become increasingly evident. For example, there are research reports that the regular use of NSAIDs may increase the likelihood cardiovascular-related mortality by up to 200%, depending on the particular product, dose, and duration of administration [Gislason et al. 2009]. Hence, along with growing usage, and for many conditions besides arthritis, there has no doubt been a continuing trend of escalating NSAID-related mortality.
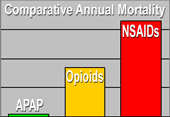
Based on the data above, the graph at left shows a proportional comparison of annual mortality attributable to APAP, opioids, and NSAIDs (using the most conservative number). Clearly, NSAID-related mortality might be of much greater concern than the other two classes of analgesics. Therefore, it is puzzling that the FDA is focusing on promoting further restrictions and controls on APAP and opioid products; an initiative that, if successful, could have unintended consequences of driving a shift toward increased use of NSAIDs with concomitant rises in mortality. Deaths associated with any medications are of great concern and worthy of ameliorative measures; however, would it make more sense to first examine the largest sector of mortality — NSAIDs — with a goal of developing better education and safety measures?
Newly Recognized Risks
There have been recent controversies about the benefits of low-dose daily aspirin (usually 81 mg/day) as antithrombotic therapy for preventing heart attack or stroke [Mathews 2010; Ong et al. 2009]. Although possibly appropriate in high-risk individuals, there are still dangers of GI complications with such therapy, particularly in the elderly, and the relative benefits in men versus women need further elaboration. In one retrospective, large-scale investigation of medical records, patients taking daily low-dose aspirin combined periodically with either ibuprofen or naproxen had up to a 3-fold increased risk of GI problems [Ivanhoe 2005]. And, there is recent evidence that COX-2 inhibitors undermine the anticlotting benefits of daily low-dose aspirin if they are taken in combination [blogpost here]; conversely, the gastroprotective benefits of COX-2 inhibitors are partially or totally lost if aspirin is used concomitantly for cardiovascular prophylaxis [Ong et al. 2009].
Furthermore, hearing loss attributed to non-opioid analgesic use has recently come to light [Curhan et al. 2010]. Writing in the American Journal of Medicine researchers reported on a survey of nearly 27,000 men, repeated every 2 years from 1986 to 2004. About one-fourth of the men had been diagnosed with hearing loss and those who used non-opioid pain relievers at least twice weekly were more susceptible than nonusers: aspirin users were 12% more likely to have hearing loss, those taking other NSAIDs were 21% more likely, and users of acetaminophen were 22% more likely. Compared with nonusers, men younger than 50 years old at the start of the study faced an even greater likelihood of hearing loss, and regular combined use of more than one type of non-opioid analgesic as well as longer duration of such use had a further negative impact on hearing. Although hearing loss is a relatively innocuous adverse effect compared with life-threatening GI and cardiovascular complications, it is noteworthy that new problems associated with non-opioid analgesics are still being discovered.
Managing Risks, Enhancing Analgesic Therapy
Judging by available evidence it seems apparent that the concept of “safe analgesia” may be an oxymoron; some risks can be managed but all of them cannot be avoided. And, the omnipresence of NSAIDs in society and cavalier attitudes toward their use may be serious deterrents to risk mitigation. Surveys have indicated that 8 out of 10 Americans use OTC NSAIDs to some extent each year; however, most of those persons (up to 60%) either are not aware of any risks or are not concerned about potential adverse events [Wilcox et al. 2005]. Consequently, more than 4 of 10 users (44%) take greater doses than recommended on the warning labels and 22% falsely believe alerting symptoms will always precede any NSAID-induced complications.
An excellent evidence-based overview by Ong and colleagues [2007, available here] discusses balancing NSAID benefits and risks. Evidence for NSAID effectiveness in treating many acute and chronic pain conditions is highly favorable, with higher-dose oral NSAIDs often outperforming comparably-dosed opioid analgesics or acetaminophen for short-term relief of acute pain [also see, Bandolier 2003]. However, there are unresolved questions about the safety of NSAIDs for treating chronic pain conditions, and adverse GI or cardiovascular events associated with NSAIDs often result in benefit-to-risk ratios favoring acetaminophen or opioid analgesics.
A further complication is that risk-mitigation strategies for using NSAIDs most effectively and safely are complex, somewhat controversial, and still being determined [Ong et al. 2007]. There are currently no comedications for reducing the cardiotoxic effects of NSAIDs. Naproxen has been viewed as somewhat less cardiotoxic but it may confer up to a 3-fold greater risk of GI complications than other NSAIDs. COX-2 inhibitors are considered as having greater GI tolerability but there have been cardiotoxicity concerns with these agents.
Four classes of drugs are available as co-therapy for reducing GI toxicity with traditional oral NSAIDs: proton pump inhibitors (PPIs), histamine H2-blockers, antacids, and prostaglandins (eg, misoprostol). The decision to initiate such co-therapy is dependent on several factors, including increased risks of serious GI complications in the following groups: [see, Ong et al. 2007; Risser et al. 2009].
- Patients with a prior history of peptic ulcer disease,
- those taking corticosteroids or anticoagulants,
- patients adjunctively taking aspirin as antithrombotic therapy,
- patients over the age of 65.
Prior peptic ulcer disease and age have been noted as the strongest predictors of absolute risk. In fact, updated guidelines from the American Geriatrics Society [2009] have nearly eliminated any recommendation of NSAIDs or COX-2 inhibitors in the elderly; rather, they strongly favor opioid-analgesic therapy for elderly patients with moderate-to-severe pain or diminished quality of life due to pain of any intensity.
In sum, NSAIDs are effective for relieving many types of pain but they carry a heavy burden of risk as demonstrated by the considerable evidence of their GI and cardiovascular adverse effects and consequent high rate of associated fatalities. This points toward a need for greater public education on NSAID hazards and better practitioner training on therapeutic strategies to help minimize risks. Acetaminophen, opioids, and opioid/non-opioid combination medications offer alternative and often better solutions for achieving effective analgesia, without the attendant problems of NSAIDs; however, these medications also carry risks that must be managed. It is important that all options are retained and remain widely available. If proposed FDA regulatory actions are realized — resulting in diminished access to and/or availability of acetaminophen and opioid products — along with a reluctance to rely on NSAIDs as awareness of their risks grows, there would be fewer analgesic choices available. The outcome might be an unprecedented American public health crisis in terms of human suffering and morbidity. What’s your opinion? Comment below.
[Postscript: To keep this blogpost brief, many discussion points have been greatly condensed. For readers interested in learning more, key points are referenced with direct links provided to full documents or, at least, to published abstracts. Links have been coded to open documents in a new browser window, so access to this page will not be lost if you take “side trips” to examine the background resources. — SBL]
UPDATE ADDENDUM: According to yet another source — U.S. CDC, National Center for Health Statistics [available here, p. 6] — opioid analgesic deaths in 2005 were nearly 11,000 and increased to about 13,800 in 2006. This is in contrast to the 8,500 deaths in 2005 reported by the National Drug Intelligence Center [NDIC 2009], noted above (ref. below), and exemplifies the inconsistencies in data reported by various government agencies. At the same time, however, it is very conservatively estimated that NSAID-related deaths have increased to 20,000 or more per year in the U.S. [see CLAAD document, p. 2]. Although there are probably biases inherent in all of the data, it still seems evident that NSAIDs may pose a significantly greater threat to public health than opioids.
REFERENCES: (also see links within the text)
> AGS (American Geriatrics Society). Pharmacological Management of Persistent Pain in Older Persons. J Am Geriatr Soc. 2009 [available here].
> Bandolier (Evidence-Based Health Care). Acute Pain. 2003 [PDF here].
> Curhan SG, Eavey R, Shargorodsky J, Curhan GC. Analgesic use and risk of hearing loss in men. Amer J Med. 2010;123(3):231-237 [ (March 2010) [article here].
> Gislason GH, Rasmussen JN, Abildstrom SZ, et al. Increased mortality and cardiovascular morbidity associated with use of nonsteroidal anti-inflammatory drugs in chronic heart failure. Arch Intern Med. 2009;169(2):141-149 [abstract here].
> Ivanhoe. Presentation at the 70th Annual Scientific Meeting of the American College of Gastroenterology; Honolulu, Hawaii; October 28 – November. 2, 2005. Ivanhoe Medical Newswire. 2005(Nov 1) [archive access requires subscription].
> Machado LAC, Kamper SJ, Herbert RD, Maher CG, McAuley JH. Analgesic effects of treatments for non-specific low back pain: a meta-analysis of placebo-controlled randomized trials. Rheumatology 2009;48(5):520-527 [abstract].
> Mathews AW. The danger of daily aspirin. Wall Street Journal. 2010(Feb 23) [available here].
> NDIC (National Drug Intelligence Center). National Prescription Drug Threat Assessment 2009 [executive summary]. 2009(Apr) [available here].
> Ong CKS, Lirk P, Tan CH, Seymour RA. An evidence-based update on nonsteroidal anti-inflammatory drugs. Clin Med Res. 2007;5(1):19-34 [PDF here].
> Risser A, Donovan D, Heintzman J, Page T. NSAID prescribing precautions. Am Fam Physician. 2009;80(12):1371-1378 [available here].
> Wilcox CM, Cryer B, Triadafilopoulos G. Patterns of use and public perception of over-the-counter pain relievers: focus on nonsteroidal antiinflammatory drugs. J Rheumatol. 2005(Nov);32(11):2218-2224 [article here].
> Wolfe MM, Lichtenstein DR, Singh G. Gastrointestinal toxicity and nonsteroidal antiinflammatory drugs. NEJM. 1999;340(24):1888-1899 [abstract here].
